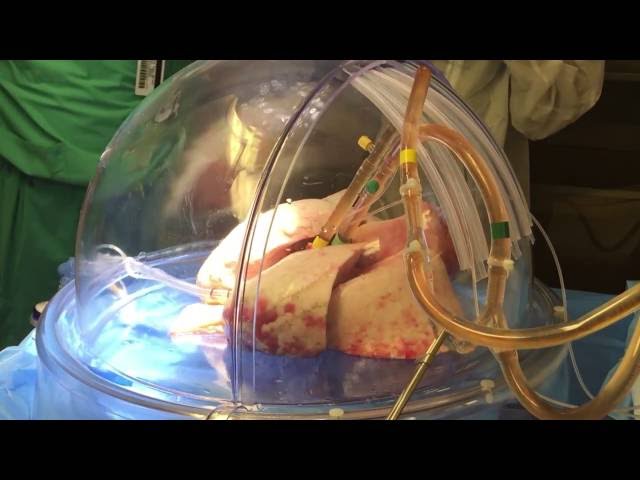
Lung Transplant Candidates
Lung Transplant Candidates
- Alpha-1 antitrypsin deficiency (AAT deficiency): an inherited condition that raises your risk for lung and liver disease. Alpha-1 antitrypsin (AAT) is a protein made by the liver that protects the lungs. If the AAT proteins aren't the right shape, they get stuck in the liver cells and can't reach the lungs.
Symptoms of AAT deficiency include:- Shortness of breath and wheezing
- Repeated lung infections
- Tiredness
- Rapid heartbeat upon standing
- Vision problems
- Weight loss
Some people have no symptoms and do not develop complications. Blood tests and genetic tests can tell if you have it. If your lungs are affected, you may also have lung tests. Treatments include medicines, pulmonary rehab and extra oxygen, if needed. Severe cases may need a lung transplant. Not smoking can prevent or delay lung symptoms.
- Bronchiectasis: The bronchi are two tubes that branch off the trachea, or windpipe. The bronchi carry air to your lungs. Common problems of bronchi include:
- Bronchiectasis, a condition in which damage to the airways causes them to widen and become flabby and scarred
- Exercise-induced bronchospasm, which happens when the airways shrink while you are exercising
- Bronchiolitis, an inflammation of the small airways that branch off from the bronchi
- Bronchopulmonary dysplasia, a condition affecting infants
- Occupational lung diseases: are caused or made worse by your work environment. They occur from inhaling dusts, chemicals or bacteria and molds at work.
The major groups of occupational lung diseases are:- Work-related asthma
- Lung disease from dusts and metals
- Allergic problems
- Reactions from irritants
- Lung or other cancers
- Infections
- Lymphangioleiomyomatosis (LAM): is a rare lung disease that mostly affects women of childbearing age. In LAM, abnormal, muscle-like cells begin to grow out of control in certain organs or tissues, especially the lungs, lymph nodes and kidneys. Over time, these LAM cells can destroy the normal lung tissue. As a result, air can’t move freely in and out of the lungs. In some cases, this means the lungs can’t supply the body’s other organs with enough oxygen.